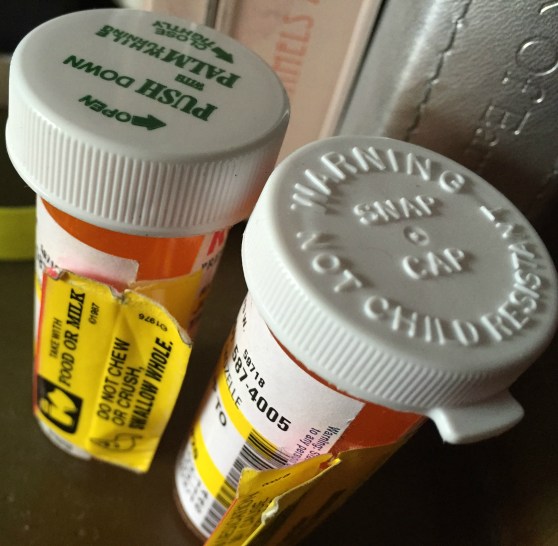
 In the Guardian this week, HRH Prince Charles proposed homeopathy as a solution to antibiotic resistance, citing his “agro-ecological” farm as an example of one that has cut antibiotic use by using homeopathic treatments.
In the Guardian this week, HRH Prince Charles proposed homeopathy as a solution to antibiotic resistance, citing his “agro-ecological” farm as an example of one that has cut antibiotic use by using homeopathic treatments.
Given the concern over bacterial resistance to medically-important antibiotics, it is vital that we find alternatives. Yet they also must have a biologically sound mode of action and be proven to be effective. It is difficult to conceive how a solution so dilute that not one molecule of active ingredient remains, where the premise of the mode of action depends on water having a “memory” of the ingredient (as opposed to all the other contaminants within that water), can possibly have any verifiable impact on disease. Indeed, there are no studies to date that show positive, replicable effects of homeopathy compared to conventional treatment.
Personally, I have no issue with any alternative therapy has been shown to be an effective alternative to conventional drugs (note that homeopathy does not fall into this category). When I underwent chemotherapy for breast cancer, I had some reiki sessions. Did I believe that energy was being channeled by the reiki healer and making me better? Honestly, no. Would I have ever considered giving up the chemotherapy? Absolutely not. But the focused breathing and relaxation certainly helped with pre-chemo anxiety. Would taking Rescue Remedy or a similar homeopathic preparation have helped? If I’d believed that it would – yes, probably. But that is biased by the placebo effect – it’s not the same as the treatment being independently effective. One of the claims made for using homeopathic treatments in animals is that they are independent of the placebo effect – they don’t have the expectation that the tincture administered is going to cure their lameness or mastitis. Yet when we assess the results, it’s not the animal who’s reporting the success or failure of the homeopathic treatment, it’s the farmer.
So let’s examine a scenario. A farmer has two mildly sick cows (e.g. slightly lame, or unwilling to eat with a raised temperature) within the herd. Both are moved to the hospital pen, given fresh bedding, water and feed plus a homeopathic remedy. Cow A gets better – hoorah for homeopathy! Cow B doesn’t and has to be treated with antibiotics – boo! Does this mean homeopathy works in 50% of cases? No. There’s no control treatment here, no evidence that Cow A wouldn’t have got better without homeopathy – some diseases just need time, TLC and the cow’s own immune system for recovery. Did the farmer cut antibiotic use? Yes – Cow A didn’t receive it. Yet again there is no evidence that this is due to the homeopathic treatment. How many times have we as humans debated whether to go to the doctor because of a minor ailment, then have found that it’s cleared up without medical treatment? It’s not miraculous, it’s simply our immune systems functioning as they are intended to.
In the absence of controlled experiments that compare homeopathic treatments to both conventional antibiotics and no veterinary treatment (save for good animal husbandry), it is disingenuous to claim that homeopathy is successful in treating bacterial disease or can effectively be used to replace antibiotics. We need to look to veterinarians and scientists when making decisions about animal care and treatment rather than relying on anecdotal data from those with royal connections. After all, HRH Prince Charles may have reduced antibiotic use on his farm, but I can also claim to have reduced antibiotic use in my household through dairy consumption – my toddler has a serious cheese addiction and has never had to take antibiotics. Hoorah – cheese is the new homeopathy!!*
(*obviously I am being sarcastic here for those who missed it, though the extent of cheese consumption and fact that she’s never had antibiotics are both entirely true)
Scare Tactics – Why Do So Many “Public Health Experts” Promote Fear vs. Food?
 How many of us are motivated by fear every single day? We’d like to think that we’re lucky enough to live in a society where we don’t feel afraid. In contrast to inhabitants of many war-torn regions we are unlikely to be shot as we drive to work; when we’re sick we have the luxury of modern medical attention (Obamacare not withstanding); and we can buy almost any food we fancy, at any time of year and feel safe in our food choices… or can we?
How many of us are motivated by fear every single day? We’d like to think that we’re lucky enough to live in a society where we don’t feel afraid. In contrast to inhabitants of many war-torn regions we are unlikely to be shot as we drive to work; when we’re sick we have the luxury of modern medical attention (Obamacare not withstanding); and we can buy almost any food we fancy, at any time of year and feel safe in our food choices… or can we?
Food safety is an underlying assumption of dietary choice within the USA. We buy food based on three major factors: taste, price and nutrition. Safety isn’t a defining factor in choosing between the cheese quesadilla, the chef’s salad or the T-bone steak because most of us have rarely experienced significant negative health effects as a consequence of food choice (aside from the annual Thanksgiving food coma).
Yet so many food commentators, self-proclaimed experts (I read Michael Pollan therefore I am…) or bloggers appear to exist for the sole purpose of instilling consumer fear. Take this recent article in Salon – 9 reasons why we should fear eating steak – apparently it’s riddled with antibiotics, full of heavy metals and likely to give us all mad cow disease. I’m not going to turn this blog post into a thesis, so today will simply address one of the issues raised in the article, and examine the others in future posts.
I’m a scientist by training. In my career to date, I’ve learned that the more controversial the topic, the more important it is to base claims on sound data that is peer-reviewed and published in order to gain trust. If I present data that challenges perceptions, the first questions are always “Is this published in a peer-reviewed journal? Who funded it? How do I know it’s correct?” That is not to say that science is the only way to communicate – it’s not. Yet when making claims, it’s important to have science, or at least logical and biologically-feasible arguments, to back them up.
Yet, if we’re asking a question, even if it’s a loaded question that may instill fear or doubt into the reader, apparently scientific foundation is redundant. Could combining coffee and bagels in the same meal cause impotence? Is breast cancer caused by the rise in popularity of household pets sleeping on their owners’ beds? Is your tiredness really the result of too little sleep, or could it be all the chemicals that “big food” uses every single day? Hey, I’m just asking! Not making a claim, not saying that X + Y = Z, just throwing the thoughts out there. But having read them, how many of us now are thinking about our sexual performance, the potential ill-effects of Fluffy the cat, or how we really do seem to be more tired nowadays? (note that these really are examples that I have invented, I know of no scientific foundation for any of them).
Possibly the most damaging line in the Salon article contained no data. No scientific foundation. Just a question:
Could Ractopamine, added to the food supply in 1997 with little public awareness1, be contributing to skyrocketing rates of obesity and hyperactivity in children?
The FDA approved the use of Ractopamine in swine in 1999. It’s added to the diet of finishing pigs, improving feed efficiency and partitioning more feed nutrients into lean meat rather than fat (as demanded by today’s consumer). Effectively it allows us to produce more pork using fewer resources, but it has been linked to behavioral changes in pigs.
Most of us are aware that childhood obesity is a huge issue (pardon the pun). Many of us know children that have been diagnosed as having attention deficit hyperactivity disorder (ADHD). So does Ractopamine cause these? It’s as likely as suggesting that eating alfalfa hay is going to make us lactate like dairy cows.
Maximum residue limits (MRLs) exist to make sure that there are no human physiological effects of veterinary drugs in meat, milk or eggs from treated animals. Regulatory bodies including CODEX assess potential human effects of a drug residue in animal products by multiplying the average residue level in food by the average intake. For example, if the residue level is 2 micrograms per 100 grams and the average person eats 300 grams of that food each day, the intake would be 6 micrograms. This intake is then compared to the acceptable daily intake (ADI) – the quantity that could be eaten every day for a lifetime without human health risk. This is usually the intake that would have a physiological effect, divided by a safety factor of one hundred. The MRL for Ractopamine in meat is 0.25 parts per million (0.00000025 grams per gram) with an ADI of 1.25 micrograms per kg of bodyweight per day.
If we examine the average pork intake for a 10 year old child in the USA (detailed calculation below) we see that they’d have to eat 13.3x more pork than the daily average to even equal the ADI – remember that’s the intake at which we would expect no physiological effect. For Ractopamine to have a physiological effect, the ADI would have to be increased one-hundred-fold. So the average 10-year old child would have to eat 1,330x more than the average child’s intake of pork, equivalent to 35 lbs of pork per day, every single day (the average adult only eats 48 lbs of pork in a year), for Ractopamine to have a health effect. My little nieces adore pork sausages, but they are pushed to eat two (approx 2 oz) in a day, let alone 35 lbs worth!
Still think that we can link Ractopamine use to obesity and ADHD? We can’t prove a negative, but it’s as tenuous a link as suggesting that we could drown in a single drop of water. So why are public health “experts” like Martha Rosenberg using fear tactics to scare us rather than extolling the positive contributions that high-quality animal proteins make to the human diet? Surely there’s no agenda there….is there?
1Note that all the data relating to this is freely-available on the internet – the “little public awareness” line is simply more fear-mongering.
Details of Ractopamine calculation
Let’s examine an average child’s intake. The average 10-year-old boy in the USA weighs 32 kg (71 lbs) and needs 34 grams of protein each day. In the USA, meat contributes about 40% of protein intake and about 21% of that comes from pork. That means, on average, a 10-year-old boy would eat about 12 g of pork per day (2.9 g protein).
If Taylor eats 12 g of pork each day at the maximum residue limit of Ractopamine (note that this would be unusually high), he’s consuming 12 g x 0.25/1,000,000 = 0.000003 g Ractopamine. His ADI = 1.25 micrograms x 32 kg bodyweight = 40 micrograms, or 0.00004 grams. That’s 13.3x higher than his intake. So a child could eat 13.3x more pork than average, every single day, and not be expected to have any physiological effects. For ingested Ractopamine to have a physiological effect he would have to eat 100 times that amount – 16 kg, or 35 lbs of pork per day. To put that into context, the average adult eats 48 lbs of pork in a year.